Rheumaderm
A Culture of Caring
Comprehensive Care for Rheumatology and Skin Health
Empowering lives through advanced medical solutions and compassionate care
Discover personalised, expert care at Rheumaderm, where advanced treatments meet a culture of compassion. From managing chronic joint pain to rejuvenating your skin, we’re dedicated to enhancing your well-being under one roof.
Contact Us
Open Hours
Monday 10 am to 8 pm
Tuesday 10 am to 8 pm
Wednesday 10 am to 8 pm
Thursday 10 am to 8 pm
Friday 10 am to 8 pm
Saturday 10 am to 8 pm
Sunday 11 am to 2 pm

about us
Meet the Experts Behind Rheumaderm
At Rheumaderm, our mission is to deliver comprehensive care in rheumatology and dermatology with empathy and expertise. Guided by Dr. Rahul Ladda and Dr. Sneha Ladda, our clinic blends cutting-edge technology with a personalised approach to improve your quality of life.
Expert Care for Your Health Needs
Explore a wide range of specialised treatments
Rheumatology Treatments:
Holistic management of arthritis, Connective Tissue Disorder (CTD), vasculitis, and osteoporosis.
Arthritis
Connective Tissue Disorder (CTD)
Vasculitis
Dermatology Treatments:
From cosmetic treatments like Medifacial and chemical peels to managing skin conditions like eczema and Lasers disorders.
Medifacial
Chemical Peels
Lasers

Why Choose Us
What Sets Rheumaderm Apart?
Expert Doctors with Years of Experience
Comprehensive Rheumatology & Dermatology Services
State-of-the-Art Equipment and Advanced Treatments
Compassionate and Patient-Centred Care


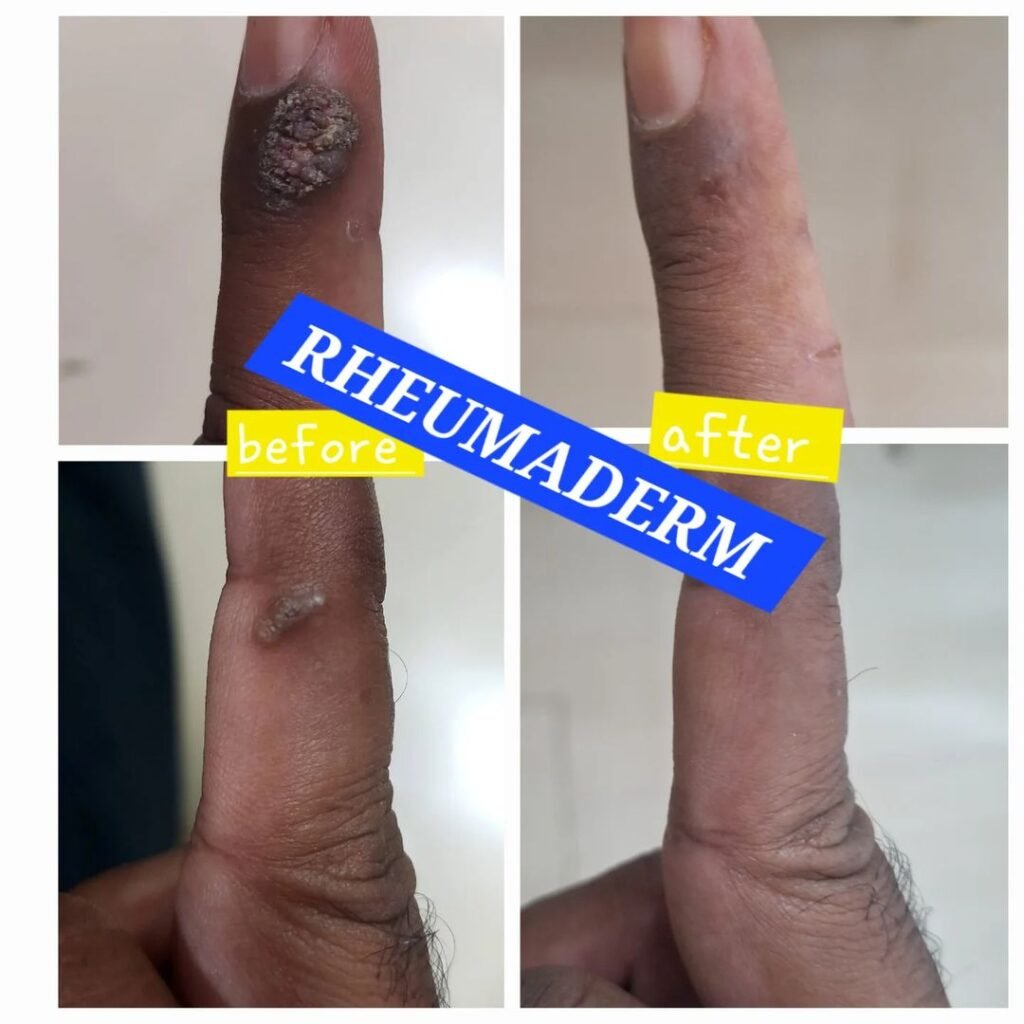
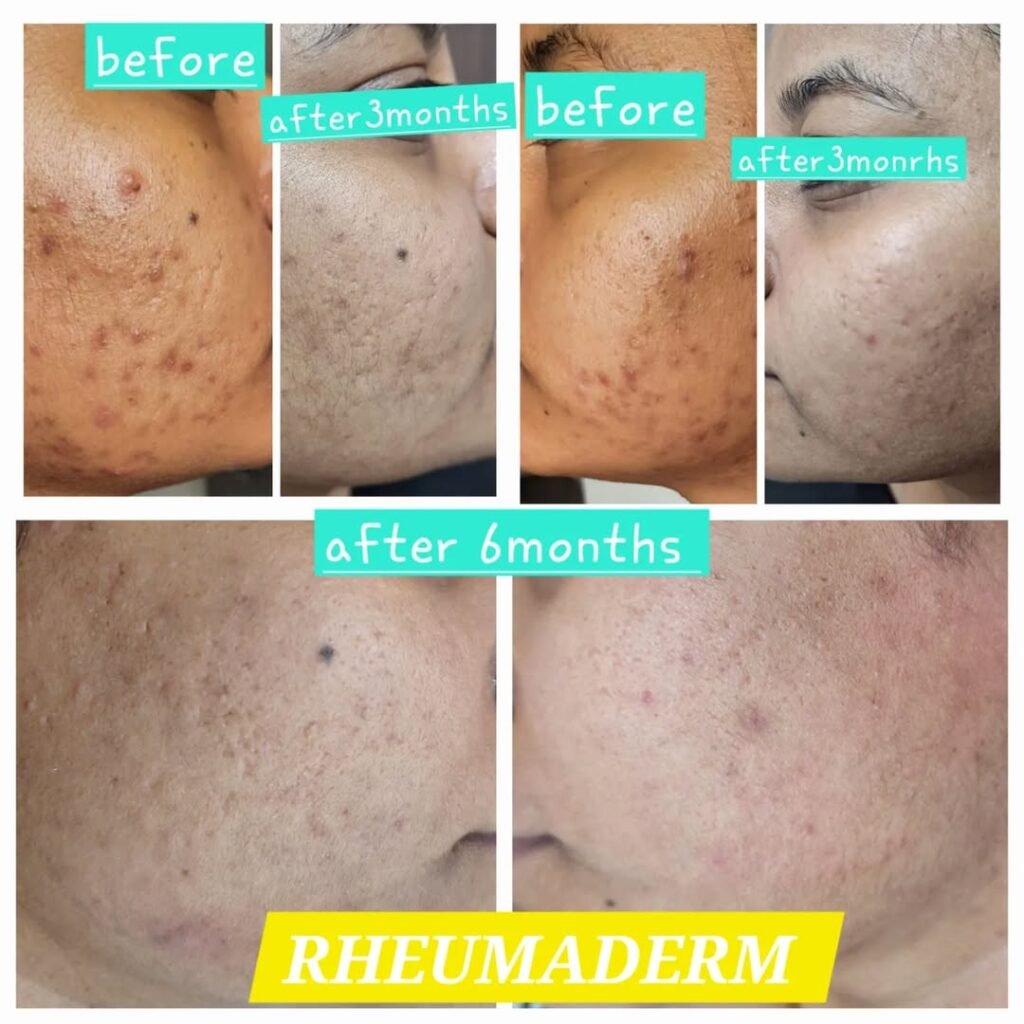
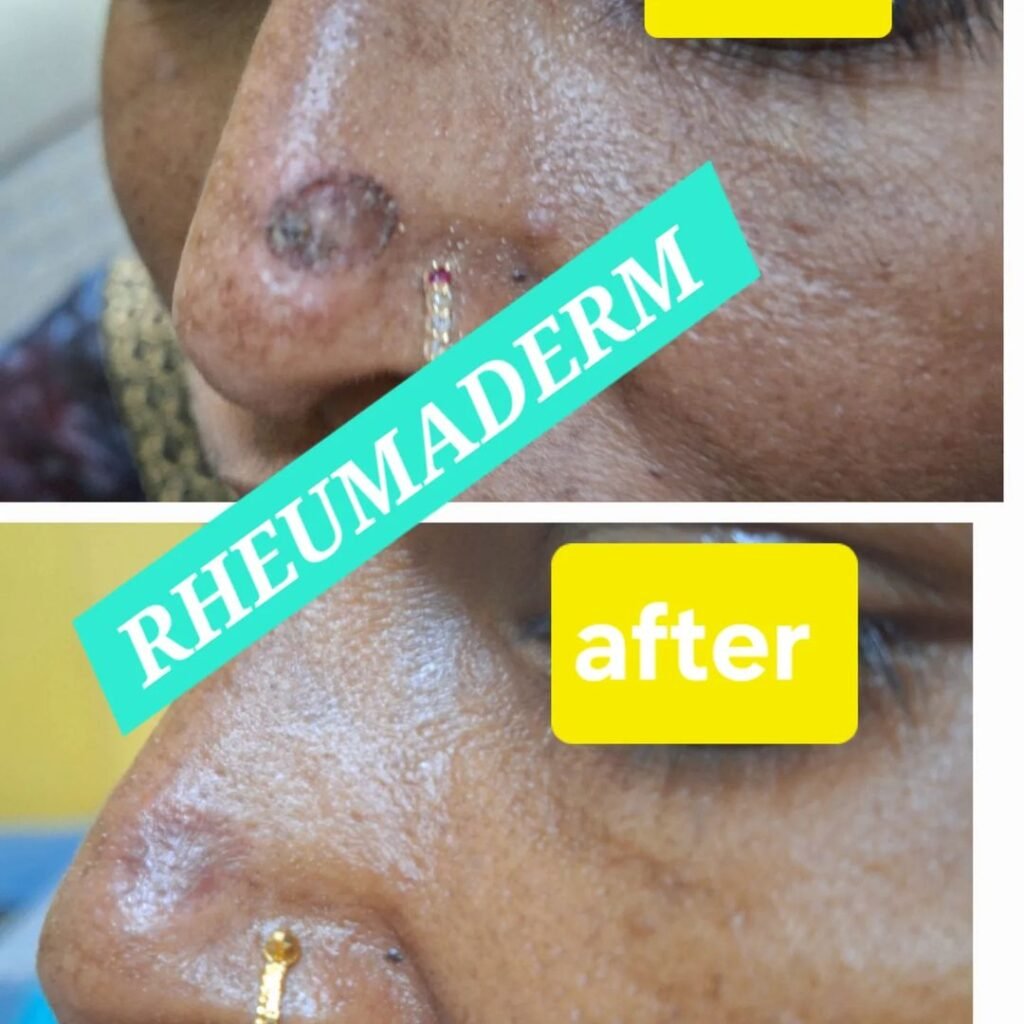
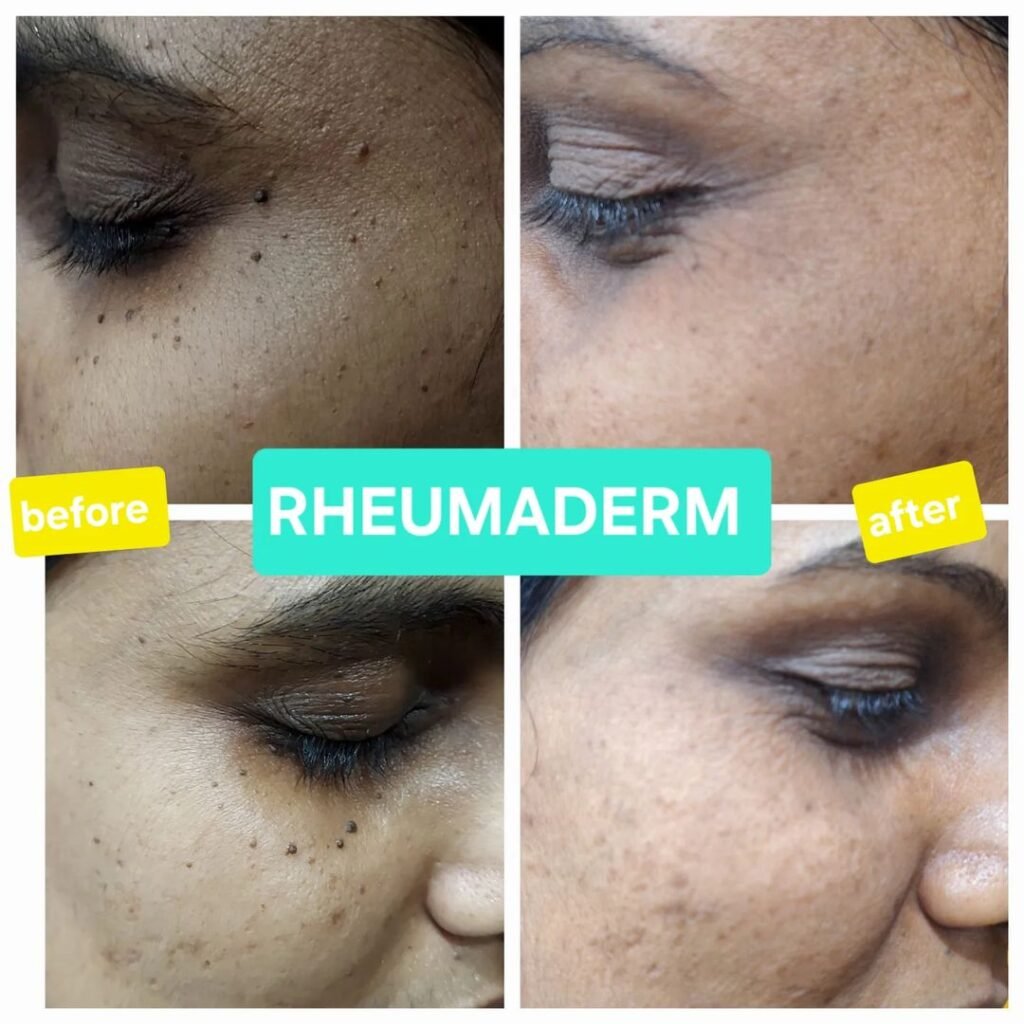
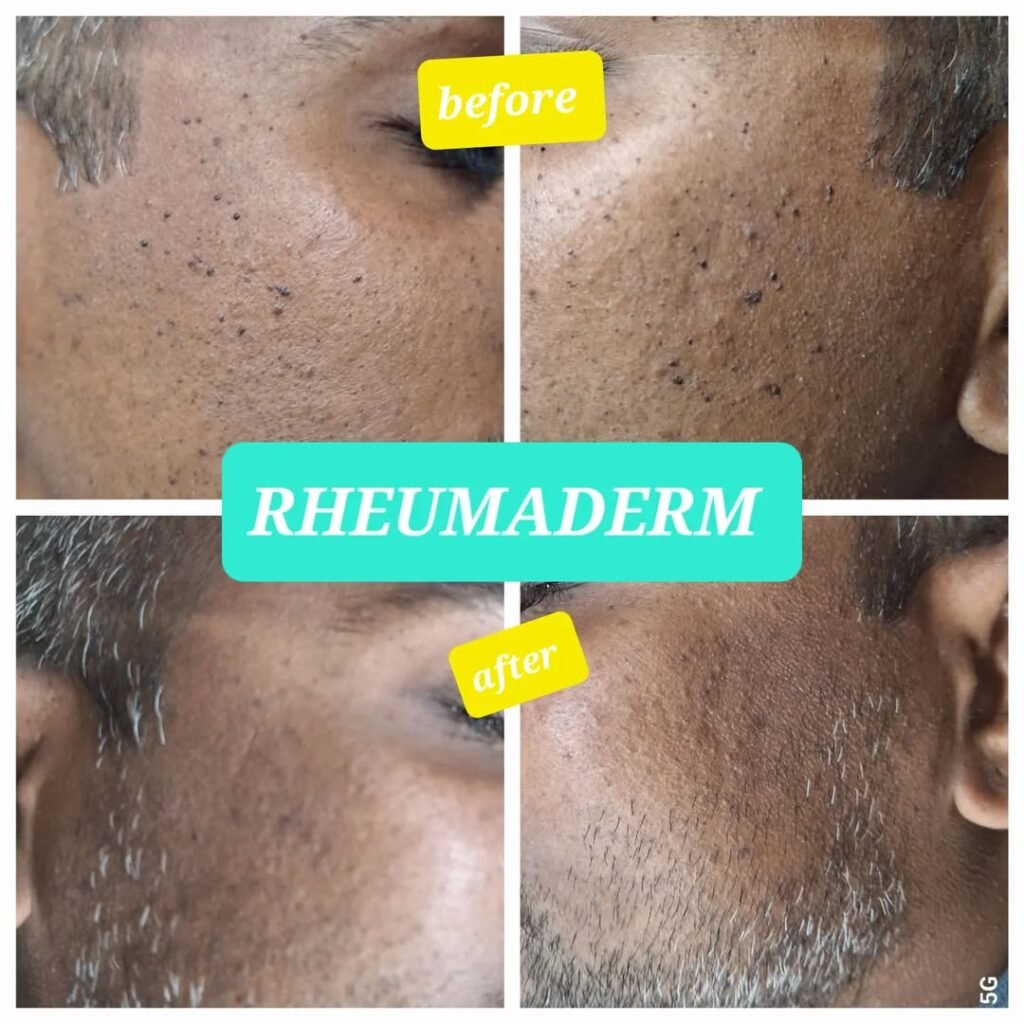
Our Results
Book your appointment at Rheumaderm
Experience personalized, compassionate treatment tailored to your needs.